In the last blog post, I went over a common pregnancy complication called gestational diabetes. This post is going to cover another common complication, preeclampsia. Scientists are not 100% sure what causes preeclampsia, but they believe it occurs when the placenta is not developed correctly. This causes blood vessels that go to the placenta to constrict and results in high blood pressure for the mother and decreased nutrient and blood flow to the baby. (1) The decrease in blood flow can cause an underproduction of amniotic fluid (the fluid that your baby floats in while in your belly) which causes the baby to be underdeveloped and malnourished. (2) The mother and the baby’s organs can be damaged due to the decreased blood flow.
Symptoms
Preeclampsia is usually diagnosed around the 20th week of pregnancy. It can be hard to diagnose because the symptoms can mimic normal pregnancy symptoms. But the two major symptoms that will indicate preeclampsia are high blood pressure and protein in the urine. Other symptoms that may occur are: (2)
- Headaches
- Blurry vision
- Seeing spots
- Right-side abdominal pain
- Swelling (especially in hands and face)
- Shortness of breath
- Dizziness
- A decrease in urine output
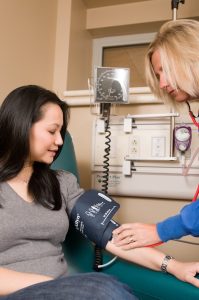
Due to the symptoms listed above being very common in a healthy pregnancy, it is important to attend all your checkup appointments with your doctor or midwife. You should be having regular urine tests and blood pressure checks at these appointments, and your healthcare provider can keep track and make sure they are within normal ranges. (1)
Effects on the Baby
As I mentioned before, the blood vessels of the placenta get constricted during preeclampsia which causes a decrease in blood flow and nutrients to the baby. This can cause the baby to have a low birth weight due to malnourishment. Preeclampsia can also cause the baby to be born prematurely and have neurological problems and learning disabilities. (2)
Risk Factors
There is no definite answer as to why some women get preeclampsia and some don’t. But there are certain risk factors that can increase a woman’s chance of being diagnosed. (1) (2)
- History of high blood pressure, kidney disease, or diabetes prior to pregnancy
- Family history of preeclampsia
- History of autoimmune diseases such as lupus or rheumatoid arthritis
- Older maternal age (over 40 years old)
- Obesity
How to Prevent
These are all great tips to keep in mind for any pregnant woman, but especially if you have one or more of the risk factors listed above. (1) (2)
- Losing weight (if needed) before pregnancy and/or maintaining a healthy weight during pregnancy.
- Exercise during pregnancy. This can help lower inflammation and help maintain a healthy weight.
- Eat a healthy diet. It is recommended to eat high-antioxidant foods like fruits and vegetables as well as potassium-rich foods to help lower blood pressure.
- Stay hydrated. Drink plenty of water and try to limit caffeine.
Treatment
If you’re diagnosed with preeclampsia, treatment will depend on how far along you are in your pregnancy. If you’re at least 37 weeks when diagnosed, you will probably be induced and/or have a C-section. If you’re earlier in pregnancy, you may be put on blood pressure medication and even bed rest for the rest of your pregnancy. (1) You will also have more checkups with your healthcare provider which could include blood tests, urine tests, and ultrasounds to make sure the baby is developing correctly. You may also receive steroid shots to help your baby’s lungs develop. (2)
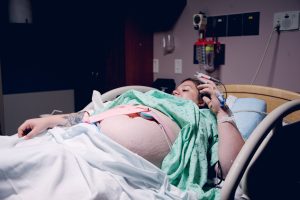
Preeclampsia is a serious condition that can lead to severe consequences for the mother and baby. While it sometimes can not be avoided, it’s important to be as healthy as possible through your pregnancy and to keep track of checkups with your healthcare provider. It’s also important to be honest and open with your healthcare provider so they are aware of your symptoms and progress through pregnancy.
If you have any questions or concerns, please contact;
Nurturing Center of Lubbock
3303 66th Street
Lubbock, TX 79413
Phone: 806-780-6853 (available 24 hours)
Text: 806-317-4480
Email: info@nurturinglife.org
Resources
- https://my.clevelandclinic.org/health/diseases/17952-preeclampsia
- https://draxe.com/health/preeclampsia/
Marlee Henn, RN
Marlee has been a nurse for two years and currently works in a functional medical clinic and part time in a long term acute care center. She has a passion for natural living, women’s health, and education.

Recent Comments